Even after COVID-19 cases fall from their current record-high levels, it's unlikely the US — let alone the world — will be able to completely eliminate the coronavirus that causes them.
But there will come a day when it's no longer a pandemic, when cases are no longer out of control and hospitals aren't at great risk of overflowing with patients.
Many experts predict that the spread of coronavirus will eventually look and feel more like that of seasonal influenza.

The US may be past the peak of Omicron cases around the end of January, some experts say; 2022 may be when the coronavirus becomes "part of our background and it comes (and) goes," Dr Ofer Levy told CNN's Alisyn Camerota this week.
"I think it's likely that we'll see this wave come and go and that the spring and summer will look a lot better than right now looks to us," the director of the Precision Vaccines Program at Boston Children's Hospital said.
"There will be fewer cases, and then again, next fall and winter we'll see a spike of viral illnesses, coronaviruses, influenza and others, but that it'll be more like an endemic cycle.
"It will be a better winter, just like this winter, with all of the challenges, is still better than the winter before."
But this coronavirus shifts and surprises frequently — and there's no official benchmark for when the pandemic has ended and a new normal has begun.
"There's not even a measurement to say that something is an epidemic or pandemic. All of this is in the eye of the beholder — and that's part of the issue," Dr Arnold Monto, a professor of epidemiology at the University of Michigan and acting chair of the US Food and Drug Administration's Vaccines and Related Biological Products Advisory Committee, told CNN in November.
"So, all of this is not based on rules. It's based typically on what you have to do to control the outbreak," he said.
"What is so different here is that our vaccines are much more effective than what we usually see."
That's the good news, according to Dr Monto. The bad news comes with the power of the virus to change and evolve.
No one can predict what the future of COVID-19 could look like — and the emergence of coronavirus variants, like Delta and Omicron, has shifted the trajectory.
"With the change in transmission patterns, as the variants have emerged — I call it a parade of variants — we now see much more extensive transmission and much more uniform spread globally. This makes declaring the end of the pandemic more difficult," Dr Monto said.
"Because the whole pattern of spread has changed, and there may still be pockets that really haven't gone through the kind of waves that the rest of the world has gone through."

'Wait and see and hold our breath'
Dr Monto and other public health leaders anticipate that in the future, the world could track the spread of SARS-CoV-2, the coronavirus that causes COVID-19, in ways similar to how the seasonal flu is monitored.
"We have no idea whether we're going to see that kind of seasonal pattern with SARS-CoV-2, but it does remind us that most of our respiratory viruses start behaving as seasonal events," Dr Monto said.
"There is the precedent for a very seasonal pattern for some of the coronaviruses that have been infecting people.
"Whether SARS-CoV-2 starts to behave like that, we don't know, but at least it gives us one scenario that it might start to behave like that."
As Dr Monto put it, we have to "wait and see and hold our breath" to unlock what an endemic phase of the coronavirus might look like.
Endemic means a disease has a constant presence in a population but is not affecting an alarmingly large number of people, as typically seen in a pandemic.
'We will get to that point where it might occasionally be up and down in the background, but it won't dominate us the way it's doing right now.'
Even in early 2020, as the pandemic was just ramping up, officials at the World Health Organisation predicted that the novel coronavirus "may become another endemic virus in our communities" and never go away.
"When you think about pandemics, you're in the pandemic phase, and then you have a deceleration phase, then you have a control phase, then hopefully you'll have elimination and maybe eradication," Dr Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, told the US Senate Committee on Health, Education Labour and Pensions at a hearing in November.
"What we hope to get it at is such a low level that even though it isn't completely eliminated, it doesn't have a major impact on public health or on the way we run our lives," Dr Fauci said.
"So if we get more people vaccinated globally and more people vaccinated now, hopefully within a reasonable period of time, we will get to that point where it might occasionally be up and down in the background, but it won't dominate us the way it's doing right now."
Even as COVID-19 cases surge to new highs, federal health officials have been thinking about how to measure the end of the pandemic and how to continue to track the coronavirus once it becomes endemic.

'There is still much to be done'
To transition from pandemic to endemic in the US, the nation has to build up immunity to the coronavirus — which means many more people need to get vaccinated, Dr Philip Landrigan, a paediatrician and epidemiologist at Boston College, told CNN in November.
With some Americans still refusing to get their COVID-19 shots and some refusing to wear masks, the transition could take more time.
About 62 per cent of the total US population is fully vaccinated against COVID-19. Even fewer have received a booster dose.
"We have to get somewhere well north of 80 per cent, possibly even well north of 90 per cent of the population with immunity, either through having had infection or through having had vaccinations," said Dr Landrigan, who worked at the CDC for 15 years.
To control the spread of the measles virus in the US population, for instance, "we had to get the immunity rate up above 95 per cent, and even then, we've had sporadic outbreaks.
"These outbreaks typically occur when you have a cluster of people in a particular place who are not immunised and all of a sudden the virus gets introduced because a traveller has come in with the virus — and bang, you've got 20 cases of measles in some town," Dr Landrigan said.
"But that's not an epidemic. It's an outbreak against a background of almost no cases or scattered endemic cases."
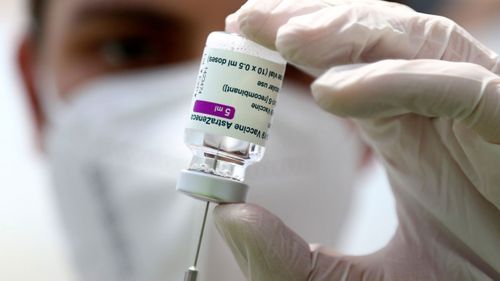
Health officials are familiar with the work needed to improve vaccination rates.
The CDC recommends that almost everyone six months and older in the US get a flu shot every year. But during the 2019-20 flu season, only about half of those people — 51.8 per cent — did, according to the CDC. The agency estimates flu has caused about 12,000 to 52,000 deaths each year between 2010 and 2020.
The coronavirus has killed more than 800,000 people in the United States so far. In the future, the battle to corral the virus every year may look very much like the annual fight against the flu.
"We've been thinking a lot about what an endemic phase looks like and the data that we're needing to collect during that phase. Certainly right now, we are collecting data on cases, hospitalisations, deaths," CDC Director Dr Rochelle Walensky said in the Senate committee hearing in November.
"The question is: What are going to be our best metrics moving forward? And probably modelling it on flu."
A more likely picture of the future
The CDC collaborates with health departments, laboratories, hospitals and health care providers to track diagnosed flu cases, determine what influenza viruses are circulating and measure the impact those viruses are having on hospitalisations and deaths.
One idea is that when the coronavirus becomes endemic, a similar tracking system could be used to monitor the pathogen.
"We could handle the cases just like we do with seasonal flu, where we're able to say we know we're going to see a number of cases in the winter season, and we can have the right staffing, we can have the right supplies ready, and we're ready to handle it, as opposed to the surges that we've been dealing with here," Dr Stephen Parodi, national infectious disease leader for Kaiser Permanente, told CNN in November.
"I'm still on phone calls talking about, 'what's our ICU bed capacity? What's our supplies chains that we need to provide care to patients? Do we have enough medication?'" Dr Parodi said.
"We have a lot more work to still do to get to where we want to be, and I think we're going to see this transition over year 2022. But for some locales, where there's less immunity, it's going to be a longer run."
Even the flu is unpredictable, and doctors have seen a lot of it over the years.
"We know there are going to be cases," Dr Monto said.
"With the flu, we've had experience with flu pandemics before. So we know typically the way they behave. This has been an evolving situation with a totally novel pathogen."
Tags:
News